The first thing Pastor Darnell Webb told me about Miguel Fulton was that he never complains. “He’ll sit in that back pew, help stack chairs after service, and not say a word about what’s going on at home,” the pastor told me when he reached out in late February 2026. “But I see it. The man is exhausted.” That was enough for me to drive out to Omaha on a gray Tuesday morning and knock on Miguel’s door.
Miguel Fulton, 54, met me at the front door of a beige split-level house on Omaha’s west side. He was still in his work clothes — a tucked-in button-down, reading glasses pushed up on his forehead. He works as an IT project manager, the kind of steady, unglamorous job that doesn’t make headlines but keeps systems running. He shook my hand firmly and offered me coffee before I even sat down.
A Raise That Came With a Hidden Price Tag
Miguel’s financial trouble didn’t start with a layoff or a medical crisis. It started with something most people would call good news. In March 2025, his employer gave him a raise — his annual salary moved from $52,000 to $61,000. With a blended family of five including his wife Sandra and three kids ranging from ages 9 to 17, that bump felt like breathing room.
“I remember thinking, okay, we can finally get ahead of things,” Miguel told me, sitting at a kitchen table stacked with mail. “We’d been stretching every paycheck for years. I thought the raise was the break we needed.”
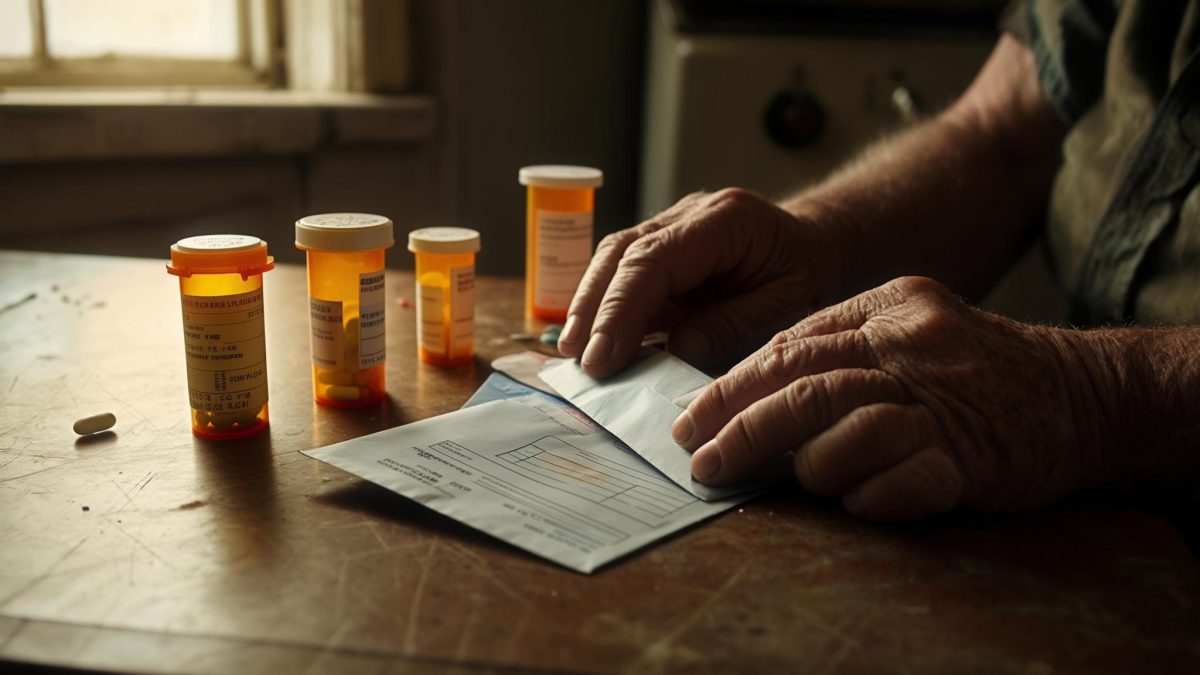
But the raise came alongside something else: his employer, a mid-size logistics firm, restructured its benefits package in January 2026. The company switched to a high-deductible health plan with a $3,200 individual deductible. Miguel, who manages Type 2 diabetes and hypertension, suddenly found that the prescriptions he’d been paying $40 a month for were now costing him $340 a month out of pocket — before he hit that deductible.
The math didn’t work. His take-home increase after taxes was roughly $480 a month. His prescription costs had jumped by $300. The raise had effectively evaporated before he could use it — and that’s before the roof.
The Roof, the Repairs, and the Debt That Quietly Stacked Up
Last autumn, a contractor told Miguel his roof had sustained significant wind damage and would need partial replacement. The estimate came back at $8,500. Miguel doesn’t have a home equity line of credit. His savings account held about $1,100 at the time. He put $2,000 on a credit card and has been making minimum payments since.
“The house is the one thing I own,” he said quietly. “I’m not going to let it fall apart. But every time I make a payment on that card, I feel like I’m just treading water.”
What Miguel described to me is a pattern that housing and health policy researchers refer to informally as the “benefits cliff” — the point at which earning more money disqualifies a household from assistance programs faster than the additional income can compensate. Nebraska expanded Medicaid under the Affordable Care Act, with full expansion taking effect in October 2020. According to Medicaid.gov enrollment data, expanded Medicaid covers adults up to 138% of the federal poverty level — for a family of five in 2026, that threshold sits at roughly $49,000 annually.
At $61,000, Miguel earns too much to qualify for Nebraska Medicaid. But not enough, it turns out, to comfortably cover chronic illness management under a high-deductible plan.
Navigating the Paperwork — and What He Found
After Pastor Webb connected him with a volunteer benefits navigator at the church, Miguel spent three weeks in February 2026 filling out applications and making phone calls. He applied for Nebraska’s Pharmaceutical Assistance Program, checked eligibility for the federal Low Income Home Energy Assistance Program, and looked into whether his children qualified for CHIP coverage separately from his own plan.
The children’s CHIP approval was the first concrete win. Under the Children’s Health Insurance Program, kids in families that earn too much for Medicaid but can’t afford private coverage can receive low-cost health coverage. For Miguel’s family, that meant his three kids — who had been on his employer’s high-deductible plan — moved to CHIP coverage with minimal cost-sharing.
“That alone probably saves us $180 a month in copays and small bills,” he told me. “The kids go to the doctor now without me having to calculate whether we can afford it.”
What Didn’t Get Fixed — and Why That Matters
I want to be honest about what Miguel’s story is not. It is not a story about a program swooping in and solving everything. When I spoke with him in late March 2026, his own prescriptions were still costing him between $180 and $220 a month — one manufacturer’s assistance program had approved him, the other had not yet responded. The roof repair was still only half-paid. The credit card balance sat at $1,740.
He had also applied for Nebraska’s Homeowner Assistance Fund, which was established using federal American Rescue Plan dollars to help homeowners with mortgage and repair costs. He was told the program had largely exhausted its allocation and that a new funding cycle was uncertain.
What Miguel described to me was not bitterness. He was precise about that. “I don’t sit around angry about it,” he said. “I just feel like I did everything right — steady job, kept the house, raised the kids — and the system still doesn’t quite reach me. It reaches people below me and people above me. Not me.”
There’s a particular kind of financial fatigue that doesn’t look like crisis from the outside. Miguel still goes to work. He still coaches his youngest son’s Saturday soccer games. He still shows up to stack chairs after Sunday service. But when I asked him whether the situation felt manageable, he paused for a long time before answering.
“Manageable,” he repeated, like he was testing the word. “Yeah. I guess manageable is the right word. Not good. Not solved. Just manageable.”
The Larger Picture Behind One Man’s Story
Miguel’s experience sits inside a much larger pattern. According to KFF health policy research, a significant share of uninsured working adults fall into coverage gaps — they earn above Medicaid thresholds but cannot afford employer-sponsored plans with high cost-sharing requirements. The switch to high-deductible plans has been widespread: the share of covered workers enrolled in HDHPs has grown substantially over the past decade, shifting more upfront costs directly onto employees.
For someone managing two chronic conditions, that shift is not an abstraction. It is $340 a month that has to come from somewhere — and in a household with five people, a crumbling roof, and a fixed income, there is not much somewhere left.
When I left Miguel’s house that Tuesday, the roof over the front porch had a patch of discolored wood I hadn’t noticed when I arrived. He caught me looking at it. “That’s from last October,” he said, with the tone of a man who has already made his peace with something he can’t fix yet.
His story doesn’t end with a triumphant resolution or a devastating collapse. It ends the way a lot of working people’s stories end — somewhere in the middle, still going, still tired, still hoping the next phone call brings better news than the last. That, too, is what navigating public assistance often looks like for people who earn just enough to be invisible to the programs designed to help them.
Related: Claiming Social Security at 62 Cost Me $312 a Month — The Permanent Penalty Nobody Warned Me About
Related: This Sacramento Uber Driver Thought She Earned Too Much for Tax Credits — She Was Wrong by $3,200




Leave a Reply